
x
A stubborn little bump that never quite heals, a flaky patch that keeps returning, or a strip of peeling skin that feels oddly sore can be easy to dismiss as dryness, irritation, or a minor breakout. Yet when these changes linger, slowly spread, or start to bleed with the slightest touch, they often raise a quiet worry that something more serious might be hiding in plain sight, especially on sun‑exposed areas like the nose, cheeks, forehead, or scalp where everyday damage quietly adds up over time.
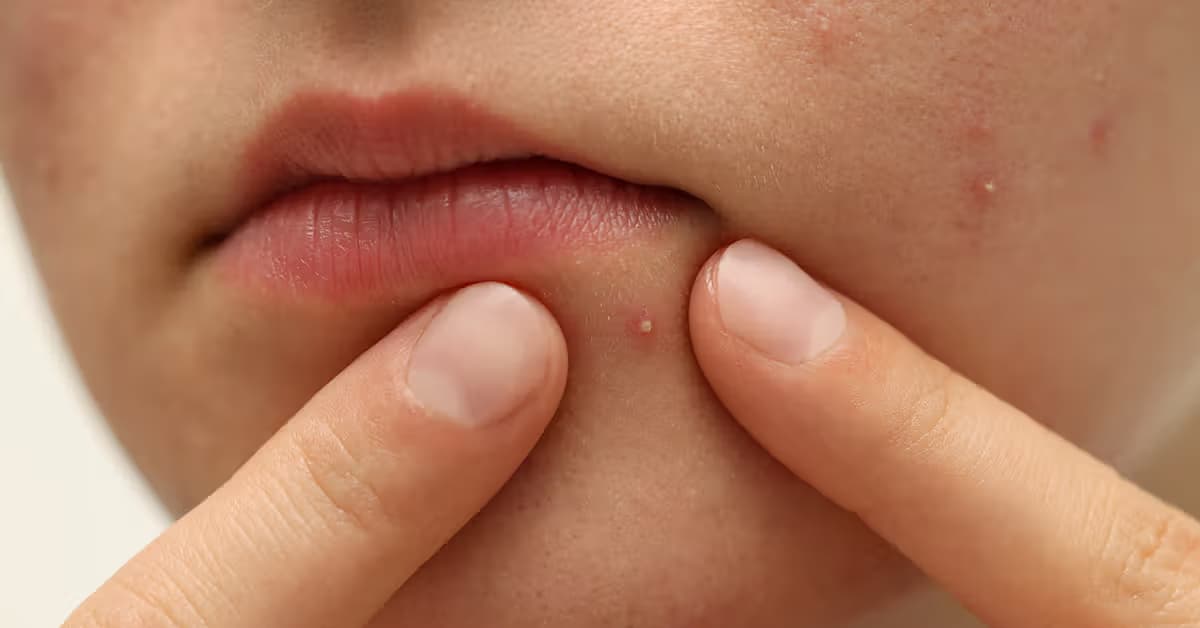
Basal cell carcinoma on the face or scalp often looks disappointingly ordinary at first. A stubborn “pimple,” a flaky red spot, or a bit of peeling skin that never quite heals can quietly grow into something much more serious if it is ignored for too long.
Basal cell carcinoma starts in the basal cells of the epidermis and is the most common type of skin cancer, especially in lighter skin tones. On the face and scalp, it often appears as a pearly bump, a red dry patch, or a small sore that crusts, bleeds, then comes back again. Nodular and superficial types usually grow more slowly and tend to stay local, but they still damage nearby skin if left alone. The real clue is persistence: anything that keeps returning to the same spot, changes in color, or gradually enlarges deserves attention.
| Situation on the face or scalp | What people often assume it is | Why a dermatologist may think about BCC instead | Practical next step for the patient |
|---|---|---|---|
| “Pimple” that has been in the same spot for weeks | Acne or irritation from cosmetics or shaving | Shiny surface, tiny visible vessels, and repeated crust‑and‑heal cycle | Track how long it has been there; book a skin check if it lasts more than a few weeks |
| Flaky red patch that comes and goes | Eczema, dandruff, or dry skin | Limited to one area, slowly widening instead of moving around | Try gentle care and sunscreen; if it persists or expands, see a dermatologist |
| Small sore that bleeds after light rubbing | Scratch from nails, glasses, or hair tools | Bleeds with minimal trauma, then never fully closes over | Photograph the spot over time; seek medical review if it looks the same or larger after several weeks |
| Waxy or pearly bump on a sun‑exposed edge (nose, ear, hairline) | “Just a mole” or age‑related change | New growth in a high‑sun area, different from other spots nearby | Ask specifically about it during a routine check‑up or schedule a focused skin exam |
Not all basal cell carcinomas behave the same. Morpheaform, micronodular, and metatypical subtypes can spread more widely under the surface, creating ill‑defined, reddish or waxy plaques that look like harmless scarring or tight skin. On the scalp, hair easily hides these subtle changes, so diagnosis is often delayed. Warning signs include asymmetry, irregular borders, shiny or pearly tones, or a lesion that keeps evolving instead of settling down. Because overall cases have increased with more ultraviolet exposure, getting any non‑healing facial or scalp spot checked early makes a big difference.
Spots on the face or scalp often feel like “just another pimple,” especially when they’re small, crusty, or easy to ignore under hair. But some of these bumps can be basal cell carcinoma, a slow‑growing skin cancer that often hides in plain sight.
Basal cell carcinoma on the face often shows up as a pink, pearly, or slightly waxy bump rather than a typical red, tender pimple. A nodular type usually looks like a shiny, dome‑shaped spot with clear borders and tiny blood vessels around the edge; it may form a small sore that never fully heals. Superficial types can be flatter, like a thin, shiny patch that keeps flaking or crusting over. When a “pimple” bleeds with very little trauma, then crusts, then comes back in the exact same place, that’s a classic warning sign to get it checked.
On the scalp, basal cell carcinoma is easy to miss because hair hides the surface. You might feel a small bump when washing or brushing, or notice dried blood on the pillow or comb without remembering any injury. Morpheaform types can look more like a pale, reddish, or whitish scar with fuzzy edges than a pimple, which makes them easy to dismiss. Any raised area that changes, bleeds easily, or slowly enlarges over weeks deserves a closer look. If a crusty spot on the face or scalp just will not heal or keeps returning, that is the moment to see a skin specialist and rule out basal cell carcinoma.
Basal cell carcinoma sounds scary, but it usually starts very quietly on the skin. Understanding why it shows up on some people more than others can turn that fear into a practical plan. Let’s walk through the everyday things—sun, skin type, habits, and history—that quietly raise the odds.
The biggest driver is cumulative UV exposure, from everyday sun plus tanning beds. BCC loves spots that catch light over and over, like the face and scalp. Fair skin that burns instead of tans, blonde or red hair, and many childhood or teen sunburns raise risk a lot, especially several blistering burns in late teens. Indoor tanning piles on more damage; in younger women it is linked with sharply higher skin cancer risk, and similar patterns show up for nonmelanoma cancers such as BCC. As UV exposure quietly adds up over a lifetime, BCC becomes more common, even in people who feel they are “careful most of the time.”
| Everyday scenario | How it might influence BCC risk in general terms | Simple adjustment that can reduce that influence | How realistic the change feels for many people* |
|---|---|---|---|
| Working or exercising outdoors most days | Gradually increases overall UV exposure to face and scalp | Use broad‑brimmed hats, sunscreen, and shade breaks during peak sun | Often achievable with planning and reminders |
| Choosing indoor tanning for appearance | Adds intense, concentrated UV on top of natural sun | Replace tanning beds with self‑tanning products and cosmetic bronzers | Can feel challenging at first but becomes easier with alternatives |
| Frequently “forgetting” sunscreen on cloudy days | Allows unnoticed UV exposure that slowly accumulates | Make sunscreen part of the morning routine regardless of weather | Usually manageable once it becomes a habit |
| Not checking the scalp or hairline at all | Makes subtle, early lesions harder to notice | Ask a partner, hairdresser, or barber to mention any odd spots | Often practical when people are comfortable asking for help |
*These statements reflect common experiences and do not predict what will happen for any one individual.
Skin tone changes how BCC looks, not whether it can appear. In lighter skin, it may show as a pearly bump, a red spot, or a crusty “pimple” that never heals. In darker skin, it can blend with surrounding color and look like a dry, scaly patch, so it is easier to miss. Getting older, having many or atypical moles, a past or family history of skin cancer, weakened immunity, or previous radiation all quietly add risk. The practical response is strict sunscreen use, shade and hats during strong sun, skipping tanning beds, and doing regular skin checks so those small crusty or red patches are found early, when treatment is simpler and scarring can be minimized.
When a small spot on the face or scalp just will not heal, it is easy to hope it is “just irritation.” For basal cell carcinoma, though, that lingering doubt is exactly the reason to get a skin expert involved early. Acting sooner usually means simpler treatment and less scarring.
Basal cell carcinoma on the face and scalp often looks like a stubborn pimple, a shiny bump with tiny blood vessels, or a dry red patch that keeps flaking or peeling. The big warning signs are persistence and change: it bleeds with light rubbing, forms a crust, then comes back in the same place, or very slowly enlarges over weeks. Because sun‑exposed facial and scalp areas carry a large share of skin cancers, any non‑healing spot in these regions deserves a closer look. In the clinic, a dermatologist examines the lesion, may use dermoscopy for extra detail, and usually recommends a quick biopsy to confirm what it is.
Once the biopsy confirms basal cell carcinoma, the next step is to match treatment to risk and location. Many small, low‑risk lesions on the face can be removed with a standard surgical excision that includes a narrow safety margin of normal‑looking skin. For higher‑risk tumors, especially near the eyes, nose, or lips, Mohs micrographic surgery offers a way to clear all cancer roots while sparing as much healthy tissue as possible. When a tumor is more extensive or growing toward the eye socket, medicines that block the hedgehog pathway can shrink it first, making later surgery less disfiguring. Newer imaging tools also help map out hidden edges so surgeons avoid taking more skin than necessary.
Q1: What exactly is basal cell carcinoma and how does it usually start on the face or scalp?
A1: Basal cell carcinoma is the most common skin cancer, starting in basal cells of the epidermis. It often begins as a pearly bump, red dry patch, or small sore that repeatedly crusts and returns.
Q2: What visual symptoms on the face or scalp should make me worry that a “pimple” might be skin cancer?
A2: Watch for a pink or pearly shiny bump with tiny blood vessels, a flat scaly patch that keeps crusting, or a sore that bleeds easily and keeps coming back in the exact same spot.
Q3: Which risk factors quietly raise my chances of getting basal cell carcinoma?
A3: Cumulative sun and tanning‑bed exposure, fair skin that burns, childhood blistering sunburns, older age, many or unusual moles, past skin cancer, weakened immunity, and prior radiation all increase risk.
Q4: When should I stop watching a spot and actually see a dermatologist about it?
A4: See a dermatologist if a facial or scalp spot doesn’t heal, keeps flaking, bleeding, or returning, slowly enlarges over weeks, or looks shiny, scar‑like, or has irregular borders and changing color.
Q5: Is basal cell carcinoma always obvious and deadly, or are there common myths I should reconsider?
A5: A common myth is that dangerous skin cancers always look dramatic. BCC often appears ordinary and grows slowly, yet can deeply damage local tissue, so subtle, persistent changes still matter and need checking.